Medical massage for head pain offers a safe, non-drug option for those whose lives are disrupted by persistent headaches. Unlike general relaxation treatments, medical massage for head pain is an evidence-informed, outcome-focused therapy that addresses the physical drivers of discomfort—including muscle tension, poor circulation, and nervous-system imbalances. This guide explores how these clinical techniques ease specific headache types and provide additional wellness gains like better sleep and improved posture for lasting relief.
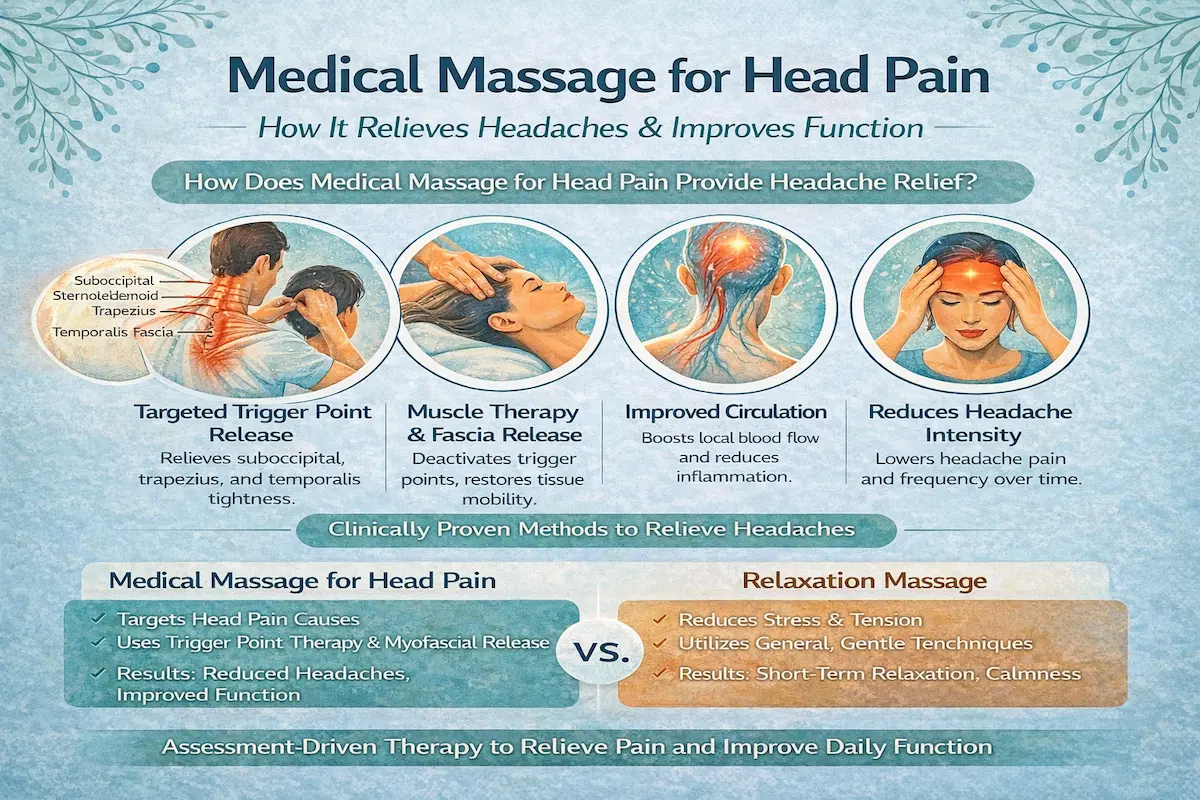
How Does Medical Massage for Head Pain Provide Headache Relief?
Treatment with medical massage for head pain begins with a clinical assessment that targets the specific anatomical and neurophysiological sources of your discomfort. By releasing tight suboccipital muscles, the sternocleidomastoid, trapezius, and temporalis fascia, clinicians use sustained pressure and fascial techniques to deactivate trigger points. This specialized application of medical massage for head pain works to restore normal tissue motion and restore structural balance.
The hands-on work involved in medical massage for head pain lowers nociceptive input to the trigeminocervical complex, boosts local circulation, and supports the body’s own pain-regulating chemistry. In practical terms, utilizing medical massage for head pain results in lower headache intensity, fewer episodes over time, and improved day-to-day function. Below, we contrast this assessment-driven method with relaxation-focused approaches to show why a clinical strategy is essential for lasting relief.
What Is Medical Massage for Head Pain and How Is It Different from Relaxation Massage?
Medical massage for head pain is goal-oriented and clinical: we assess posture, range of motion, trigger points, and pain referral patterns. Based on these specific findings, we select evidence-based techniques—such as trigger point release, deep tissue work, or myofascial release—to treat the root cause of the discomfort. In contrast, relaxation massage primarily aims to reduce general stress and promote a sense of calm.
The distinction is vital because medical massage for head pain focuses on documenting measurable outcomes, coordinating care with other healthcare providers, and correcting the physical dysfunctions that create chronic headaches. For example, when utilizing medical massage for head pain, treating suboccipital tightness with targeted trigger point therapy and home mobility exercises is a common clinical pathway used to reduce cervicogenic referral. This assessment-driven focus leads naturally into the physiological mechanisms that allow the body to heal.
What Physiological Mechanisms Help Reduce Head Pain with Medical Massage?
Medical massage eases head pain through several complementary mechanisms: mechanical deactivation of trigger points, improved blood and lymph flow, and neurochemical shifts that raise endorphins and lower stress hormones. Releasing trigger points in the temporalis or sternocleidomastoid can reduce referred head pain; improved circulation clears sensitizing metabolites; and calming the sympathetic nervous system supports restorative sleep and recovery.
Over time these effects may reduce central sensitization and help break the cycle of chronic headache. Understanding these mechanisms helps match techniques to the headache types most likely to benefit.
Which Types of Head Pain Can Medical Massage for Head Pain Treat Effectively?
Medical massage can help several common headache types when the treatment targets the primary driver. Tension-type headaches often respond to myofascial and muscle-release techniques. Migraines may improve when peripheral trigger points, sleep disruption, and stress are addressed. Cervicogenic headaches typically require neck-focused soft-tissue and joint work.
Sinus-related facial pressure can sometimes ease with lymphatic drainage and gentle facial release—though infection or other medical causes should be evaluated by a clinician. Realistic expectations are important: massage usually reduces intensity and frequency, supports medication-sparing strategies, and works best when paired with posture and lifestyle changes. The table below maps headache types to common causes and the primary massage approaches used.
Different headache types respond to specific massage strategies based on their usual triggers and tissue targets.
| Headache Type | Common Causes/Triggers | Medical Massage Approaches |
|---|---|---|
| Tension-type headache | Sustained neck/shoulder tightness, stress, poor ergonomics | Myofascial release, deep tissue techniques, scalp massage, home stretching |
| Migraine | Multifactorial: trigger points, autonomic triggers, sleep and stress disruption | Trigger point therapy, relaxation strategies, sleep-supportive sessions |
| Cervicogenic headache | Referred pain from neck joints/muscles, postural strain | Neck-focused soft-tissue work, joint mobilization, complementary modalities |
| Sinus-related headache | Nasal congestion, lymphatic stasis, facial muscle tension | Lymphatic drainage, gentle facial myofascial release, relaxation work |
This quick mapping helps you and your clinician choose appropriate techniques and set expectations about symptom relief versus prevention. The sections below describe how massage is applied for migraines, tension headaches, and cervicogenic or sinus-related pain.
How Does Medical Massage for Head Pain Help Migraines?
For many people with migraines, massage is a useful adjunct. We address peripheral triggers—tight muscles and trigger points in the neck, scalp, and shoulders—while also reducing physiological stress and supporting better sleep. Deactivating these peripheral inputs lowers overall sensitization that can amplify migraine pathways, and relaxation-focused elements reduce sympathetic arousal that often precedes attacks.
Because migraines are complex, massage works best as part of a broader plan that includes trigger tracking, sleep strategies, and medical management when needed.
What Techniques Are Used for Tension Headaches in Medical Massage for Head Pain?
Tension headaches respond well to techniques that reduce muscle overactivity and restore fascial mobility in the neck, upper back, and scalp. Long, directed strokes, focal trigger point release, deep tissue work, and myofascial release are commonly used.
Simple home care—self-massage with a tennis ball, daily neck mobility drills, and ergonomic adjustments—helps lock in improvements. Many patients notice lower intensity after a few sessions and sustained benefit when clinical care is paired with consistent at-home routines.
Can Medical Massage for Head Pain Relieve Cervicogenic and Sinus Headaches?
Cervicogenic headaches often respond predictably to focused work on the neck—suboccipital muscles, levator scapulae, and upper trapezius—to reduce referred nociception and restore mobility. Sinus-related headaches may improve with lymphatic drainage and gentle facial release, but if infection, fever, or severe congestion is present you should seek medical or ENT evaluation.
Knowing these limits helps keep massage safe and effective as part of integrated care.
What Are the Hidden Benefits of Medical Massage for Head Pain Beyond Pain Relief?
Medical massage offers benefits beyond immediate pain relief. Over time it can improve sleep quality, reduce anxiety, improve posture, and decrease reliance on pain medications. These secondary gains come from physiological changes—lower sympathetic tone, reduced cortisol, greater parasympathetic activity, and better tissue perfusion—and from behavioral effects like increased body awareness and adherence to ergonomic strategies.
Research also suggests manual therapy can improve quality of life for people with certain headache types.
Manual Therapy Can Improve Quality of Life for Headache Patients
A systematic review and meta-analysis found manual therapy may improve quality of life in people with tension-type headache and migraine, while results for cervicogenic headache were less consistent. The authors caution that evidence quality is low and recommend future studies use disease-specific, reliable outcome measures.
Manual therapy and quality of life in people with headache: systematic review and meta-analysis of randomized controlled trials, A Turolla, 2019
| Benefit | Mechanism (how it works) | Practical Outcome for Patient |
|---|---|---|
| Improved sleep quality | Reduces sympathetic tone and cortisol, increases parasympathetic activity | Fewer nighttime awakenings and more restorative sleep |
| Reduced anxiety and stress | Increases endorphins and lowers stress hormones | Fewer headache triggers and better daily coping |
| Posture correction | Releases chronically tight muscles and improves muscular balance | Less cervicogenic strain and fewer tension headaches |
| Reduced medication reliance | Lowers pain intensity and frequency through tissue and neural change | Fewer analgesics needed and fewer medication side effects |
These secondary benefits support long-term reductions in headache burden and improved daily function. If you’d like integrated local care, Messina Acupuncture combines medical massage with complementary therapies to amplify these results and help patients maintain gains.
Messina Acupuncture blends traditional Chinese medicine and modern orthopedic techniques into individualized plans that may include medical massage, acupuncture, acupressure, or dry needling when appropriate.
This integrated approach supports continuity of care and gives patients access to targeted manual therapy within a broader recovery plan.
In addition to medical massage, we offer acupressure—a gentle, non-invasive manual method that can ease headache-related tension—and dry needling for precise trigger-point work when clinically indicated.
Which Medical Massage for Head Pain Techniques Does Messina Acupuncture Offer?
At Messina Acupuncture we use assessment-driven technique selection to match treatment to anatomy and goals. Common approaches include trigger point therapy for referring nodules, deep tissue work for chronic muscle remodeling, craniosacral techniques and myofascial release for fascial restrictions, and gentle modulation when tissue tolerance is limited.
We frequently combine these methods with acupuncture or dry needling when indicated. Each session includes hands-on treatment, posture assessment, and a tailored home program with recommendations on frequency to reduce headache recurrence. The table below outlines techniques, targets, and expected outcomes so you know what to expect.
Below is a comparison of techniques, their primary anatomical targets, and typical clinical outcomes.
| Technique | Target Anatomy / Trigger Points | Expected Benefit / Outcome |
|---|---|---|
| Trigger Point Therapy | Suboccipital muscles, temporalis, SCM | Rapid deactivation of referring nodules and reduction in headache intensity |
| Deep Tissue Massage | Upper trapezius, levator scapulae, cervical paraspinals | Long-term remodeling of chronic tightness and improved neck mobility |
| Craniosacral Therapy | Cranial fascia, dural tensions, light scalp tissues | Gentle modulation of cranial tension and reduced sensitivity in tension headaches |
| Myofascial Release | Fascia of neck, shoulders, and scalp | Improved fascial glide, decreased referred pain, and better range of motion |
This inventory clarifies how we choose modalities for specific clinical presentations and helps you make informed decisions about care. To book targeted techniques locally, Messina Acupuncture accepts appointments in Setauket, NY.
What Are the Benefits of Trigger Point Therapy and Deep Tissue Massage in Medical Massage for Head Pain?
Trigger point therapy and deep tissue massage complement one another: trigger point work applies sustained pressure to deactivate referring nodules—often in the temporalis, suboccipitals, or SCM—for rapid symptom relief, while deep tissue techniques use slower, focused strokes to lengthen and reorganize chronically tight muscle fibers for longer-lasting change.
Many patients notice immediate easing after trigger point sessions and steady improvements in mobility and fewer headaches as deep tissue changes accumulate across multiple visits.
How Do Craniosacral Therapy and Myofascial Release Support Headache Relief in Medical Massage for Head Pain?
Craniosacral therapy and myofascial release are gentler, fascia-focused options for people with heightened cranial tension or sensitivity. Craniosacral work uses light-touch assessment and subtle releases to improve cranial mobility and ease dural tension that can worsen tension-type headaches or increase migraine sensitivity.
Myofascial release restores glide between fascial layers in the neck and shoulders, reducing referred pain and improving posture mechanics that perpetuate headaches. These methods are often introduced early in a graded program and progressed as tissue tolerance allows.
Why Choose Messina Acupuncture for Medical Massage for Head Pain in Setauket, NY?
Messina Acupuncture offers a patient-centered, holistic model that prioritizes targeted pain relief, functional improvement, and coordinated care. As a family-run practice, we combine hands-on experience in musculoskeletal and headache care with administrative support to help with insurance paperwork when appropriate.
What Personalized Care and Expertise Does Daniel Messina Provide in Medical Massage for Head Pain?
Daniel Messina leads care with an emphasis on individualized assessment and targeted interventions for musculoskeletal pain and headaches. Treatment plans focus on the drivers identified during evaluation—trigger points, postural imbalance, or fascial restriction—and include hands-on therapy, practical home programs, and clear outcome tracking.
The goal is to reduce symptoms while empowering patients with ergonomic and self-care strategies to sustain improvements.
How Does Messina Acupuncture Support Insurance and Flexible Scheduling for Medical Massage for Head Pain?
We help patients navigate insurance documentation and offer flexible hours to reduce scheduling barriers. Our administrative team can assist with paperwork so you can focus on care, and appointment times are arranged to fit work, family, or travel commitments.
For specific coverage details and availability, please call the clinic to discuss your situation and next steps.
How Can You Book Medical Massage for Head Pain Relief?
Below are the practical steps to schedule care in Setauket, NY or to register interest from abroad.
To schedule an appointment, follow these clear steps:
- Call to initiate care: Phone the clinic at 631-403-0504 to describe symptoms and check availability.
- Complete an intake and assessment: We document headache patterns, triggers, and prior treatments to guide targeted therapy.
- Agree on a treatment plan: Your clinician will recommend techniques, session frequency, and home exercises tailored to your goals.
- Arrange follow-up and insurance details: Staff can help with scheduling and insurance paperwork when applicable.
Frequently Asked Questions
What should I expect during my first medical massage for head pain appointment?
Your first visit includes a focused intake and physical assessment: we’ll review headache history, triggers, and past treatments, then evaluate posture, trigger points, and range of motion. Based on that assessment we’ll develop a personalized plan—techniques to use, session frequency, and home exercises.
Most initial visits include a brief hands-on treatment so you leave with a clear plan and practical strategies to try at home.
How often should I receive medical massage for head pain for optimal results?
Frequency depends on your symptoms and goals. Many patients start with weekly sessions for a few weeks to establish relief, then transition to every-other-week or monthly maintenance as symptoms improve. Your clinician will recommend a schedule based on assessment and progress—consistency in the early phase usually yields the best long-term outcomes.
Are there any side effects associated with medical massage for head pain?
Medical massage is generally safe. Some people experience mild soreness, tiredness, or a brief increase in headache intensity after treatment as tissues adjust. These effects are usually short-lived.
Tell your therapist about any discomfort so they can modify pressure or technique. For most patients the benefits outweigh temporary discomfort.
Can medical massage for head pain be combined with other treatments for headaches?
Yes. Medical massage pairs well with acupuncture, physical therapy, medication management, and lifestyle strategies. An integrated plan can address multiple contributors to headache—muscle tension, posture, sleep, and stress—so therapies complement one another.
Always coordinate with your healthcare providers to ensure a safe, effective combined approach.
How can I maintain the benefits of medical massage for head pain at home?
Home care is essential. Regular stretching, ergonomic adjustments, self-massage (for example with a tennis ball), and daily neck mobility exercises reinforce clinic work. Staying hydrated, managing stress with breathing or mindfulness, and prioritizing sleep also help preserve gains and reduce headache recurrence.
Is medical massage for head pain suitable for everyone with head pain?
Medical massage can help many people, but it’s not appropriate for every case. Severe infections, acute injuries, or certain medical conditions may require other approaches. A full assessment will determine whether medical massage is safe and likely to help in your situation.
If needed, we’ll recommend medical or specialist referral.