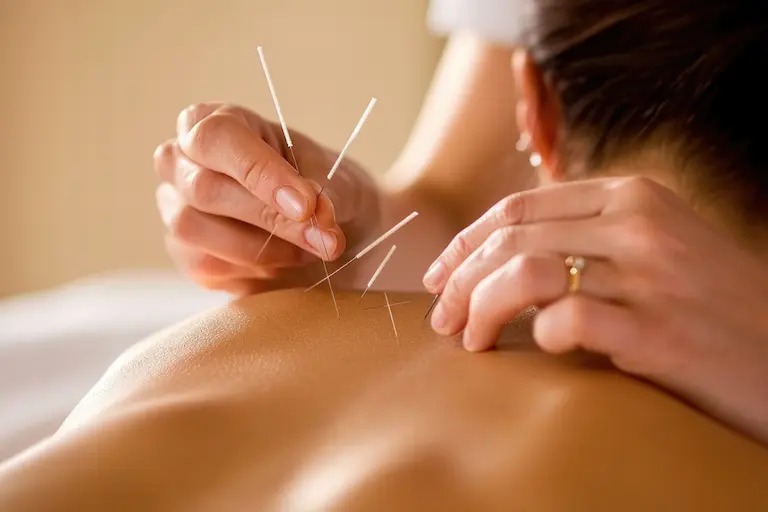
If you are living with chronic muscle pain in Setauket, you have likely navigated a confusing maze of medical advice. You visit an orthopedist for back pain, and they offer a “Trigger Point Injection.” You see a physical therapist, and they suggest “Dry Needling.” You talk to a friend at the gym in Stony Brook, and they swear by “Cortisone shots.”
For the average patient, this terminology is overwhelming. All of these therapies involve needles. All of them target pain. All of them claim to release “knots” in the muscle. So, are they the same thing?
The answer is a definitive no. While they share a target, the tools, the physiological mechanisms, and the long-term effects on your tissue are radically different.
At Messina Acupuncture, we believe that an informed patient makes better health decisions. In this comprehensive, deep-dive guide, we will analyze the battle of Dry Needling vs. Wet Needling. We will look at the needle physics (solid vs. hollow), the chemicals used (or not used), and the rigorous scientific evidence supporting each, so you can decide which path is right for your recovery.
The Shared Enemy: Anatomy of a “Trigger Point”
To understand the treatment, you must first understand the problem. Both therapies target Myofascial Trigger Points. But what exactly is a “knot”? It isn’t just a metaphor; it is a distinct physiological event known in medical literature as the “Integrated Trigger Point Hypothesis.”
The Physiology of Pain
Your muscles are made of millions of microscopic fibers called sarcomeres. These fibers slide past each other to contract and relax. A trigger point occurs when this system jams.
- The Chemical Leak: Due to repetitive stress (like typing all day) or acute injury, the nerve ending releases too much Acetylcholine. This chemical tells the muscle to contract.
- The Calcium Flood: This signal causes a flood of calcium ions into the muscle cell, locking the sarcomeres in a permanent state of contraction.
- The Choke (Ischemia): This tight contraction squeezes the tiny capillaries shut. Blood cannot get in (to bring oxygen), and waste cannot get out.
- The Toxic Soup: Without fresh blood, acidic waste products—specifically Bradykinin, Substance P, and CGRP—build up in the tissue. These chemicals scream “pain” to the brain.
Both Dry and Wet needling aim to break this cycle, but they use very different weapons to do it.
What is Dry Needling? (The Mechanical Reset)
Dry Needling is a technique performed by licensed acupuncturists (like our team at Messina Acupuncture) and specifically certified physical therapists. It is called “dry” because the needle is solid; there is no hollow bore to inject fluid. It relies on physics, not pharmacology.
The Tool: The Filiform Needle
We use a sterile, solid filament needle. It is incredibly thin—typically 0.25mm to 0.30mm (about the width of a human hair or a cat’s whisker). Because it is solid and has a conical, rounded tip, it separates the muscle fibers rather than cutting through them. This makes insertion significantly more comfortable than a hypodermic needle.
The Mechanism: The Local Twitch Response (LTR)
The goal of dry needling is to elicit a Local Twitch Response (LTR). When the needle enters the trigger point, it physically disrupts the dysfunctional motor endplate. This causes the muscle to twitch involuntarily, like a spinal reflex.
This twitch is the magic moment. It triggers Mechanotransduction:
- Mechanical Release: The twitch forces the sarcomeres to unlock and lengthen to their resting state.
- Chemical Flush: The twitch instantly restores blood flow (Hyperemia), flushing out the acidic “toxic soup” (Substance P) and replacing it with oxygenated blood.
- Fibroblast Activation: The physical presence of the needle stimulates fibroblasts (cells that build connective tissue) to remodel the fascia, making it stronger and more flexible.
What is Wet Needling? (The Chemical Intervention)
Wet Needling is more commonly known as “Trigger Point Injections” (TPI). This is a medical procedure performed by MDs, DOs, Nurse Practitioners, or Physician Assistants. It is called “wet” because a hollow hypodermic needle delivers a liquid substance directly into the muscle belly.
The Tool: The Hypodermic Needle
Because the needle must be hollow to allow fluid to pass through, it is significantly thicker (usually 21 to 25 gauge, or 0.5mm to 0.8mm). Crucially, it has a beveled (cutting) edge. This acts like a tiny scalpel to slice through skin and fascia. This causes more tissue trauma upon entry and is generally more painful than a dry needle.
The Menu: What Are They Injecting?
While the needle itself provides some mechanical stimulation, the primary effect comes from the drug injected. The substance determines the outcome. Here are the four most common injectates:
1. Lidocaine / Procaine (Anesthetic)
Goal: Numb the area immediately. Pros: Immediate pain relief. Breaks the pain cycle, allowing the muscle to relax. Cons: Short duration. Lidocaine is myotoxic (toxic to muscle tissue) in high concentrations and can cause temporary necrosis (tissue death) at the injection site.
2. Corticosteroids (Cortisone)
Goal: Suppress inflammation powerfully. Pros: Excellent for acute bursitis or joint swelling. Cons: Cortisone is catabolic, meaning it breaks down tissue. A landmark 2019 study published in Radiology found that corticosteroid injections can accelerate the progression of osteoarthritis and lead to joint collapse or tendon rupture. For this reason, doctors usually limit you to 3 injections per year.
3. Botox (Botulinum Toxin)
Goal: Paralyze the muscle. Pros: Used for chronic migraines or severe spasticity. Cons: Extremely expensive. It causes muscle atrophy (weakness) because the muscle is chemically prevented from contracting.
4. Saline (Salt Water)
Goal: Hydrodissection. Pros: Uses pressure from the fluid to separate sticky layers of fascia. No drug side effects. Cons: Still requires a large, painful needle.
The Showdown: A Direct Comparison
For patients in Stony Brook and Port Jefferson trying to decide, here is a direct comparison of the patient experience.
| Feature | Dry Needling | Wet Needling (Injections) |
|---|---|---|
| The Needle | Solid, flexible, hair-thin (0.3mm) | Hollow, rigid, thick (0.6mm+) |
| Sensation | Deep ache, heavy twitch | Sharp sting, burning (from fluid) |
| Drug Risk | None (100% Drug-Free) | Steroid side effects, allergies |
| Tissue Effect | Anabolic (Regenerates tissue) | Catabolic (Can weaken tissue) |
| Frequency | Can be done weekly | Limited (Steroids max 3x/year) |
| Cost | Often lower / Cash or specific codes | Higher / Medical deductible |
Does the Science Support Dry Needling?
Skeptics often ask: “If you aren’t injecting medicine, how does it work?” The answer is that the lesion is the medicine.
A 2021 Systematic Review published in Chiropractic & Manual Therapies (Sousa Filho et al.) compared Dry Needling head-to-head against Corticosteroid Injections for musculoskeletal pain. The researchers analyzed 6 randomized controlled trials and found no significant difference in pain or disability reduction between the two groups for myofascial pain.
The Takeaway: If Dry Needling provides the same relief as a steroid injection but without the risk of tissue degradation or blood sugar spikes, it is often the safer first-line choice.
Which One Should You Choose?
At our Setauket clinic, we assess patients individually. Here is a guide to which therapy wins for specific conditions.
Winner: Dry Needling
Dry needling is the superior choice for mechanical muscle dysfunction:
- Chronic Neck Pain / Headaches: Releasing the suboccipital muscles with a tiny needle is safer and more precise than injecting fluid near the skull base.
- Sciatica / Piriformis Syndrome: We can safely reach the deep glute muscles to release the pressure on the sciatic nerve without numbing your entire leg.
- Tennis Elbow / Achilles Tendonitis: Because tendons have poor blood flow, dry needling stimulates angiogenesis (new blood vessels). Cortisone here is dangerous as it weakens the tendon, increasing rupture risk.
Winner: Wet Needling
There are specific times when an injection is better:
- Acute Bursitis: If a bursa (fluid sac) is inflamed and swollen (like a grapefruit on your elbow), a corticosteroid injection is necessary to chemically suppress that inflammation fast.
- Severe Arthritis: Injecting lubricating fluid (viscosupplementation) into a bone-on-bone knee joint provides cushioning that dry needling cannot mimic.
The Safety Factor: Why Training Matters
Safety is not just about the tool; it is about the operator. In New York, the training requirements for Dry Needling are rigorous.
A Licensed Acupuncturist (L.Ac), like the team at Messina Acupuncture, must complete a Master’s or Doctorate degree involving over 3,000 hours of training. This includes extensive cadaver labs, anatomy exams, and Clean Needle Technique certification. We are experts in needle depth and avoiding neurovascular structures.
In contrast, trigger point injections are often a minor part of a general practitioner’s training. Furthermore, in some states, dry needling certification for other professions can be obtained in a weekend seminar (20–50 hours). When you are dealing with needles near your lungs (pneumothorax risk) or major nerves, experience matters.
What to Expect: A Walkthrough of Your Visit
Fear of the unknown keeps many people in pain. Here is exactly what happens during a Dry Needling session at Messina Acupuncture.
- Palpation: We use our hands to find the trigger point. It feels like a small, hard pea under the skin. When we press it, you will recognize your specific pain pattern (“Yes, that’s the spot!”).
- Insertion: We tap the filament needle in using a guide tube. You barely feel this.
- Elicitation: We gently advance the needle to the knot. You will feel a deep ache or a “crampy” sensation.
- The Twitch: The muscle jumps. This takes less than a second. It is a strange sensation, but it signals the release of the tension.
- Post-Care: We often follow up with electric stimulation or medical massage to flush the area.
Recovery: The Next 24 Hours
Wet Needling Recovery: Because of the anesthetic (Lidocaine), you often feel instant relief (numbness). However, once the drug wears off in 4–6 hours, the “rebound pain” from the large needle trauma can be significant. Cortisone flare-ups can last 48 hours.
Dry Needling Recovery: You will feel sore, similar to how you feel after a heavy gym workout (DOMS). This is a good sign—it means the muscle is remodeling. This soreness peaks at 24 hours and vanishes, leaving the muscle looser and stronger. We recommend:
- Heat: A hot bath or heating pad to keep blood flowing.
- Movement: Gentle walking keeps the muscle from stiffening.
- Hydration: Water helps flush the metabolic waste released by the twitch.
Why Setauket Residents Choose Messina Acupuncture
We pride ourselves on offering a holistic, regenerative alternative to pain management. We treat patients from Stony Brook University Hospital, local athletes, and North Shore residents who are tired of the “Band-Aid” approach of painkillers and steroid shots.
We don’t just numb your pain; we help your body fix the machinery causing it.
Read Our 5-Star Reviews on Google
Conclusion: Choose Regeneration Over Numbing
You do not always need a chemical solution for a mechanical problem. If your pain is caused by tight, dysfunctional muscle fibers, Dry Needling offers a direct, safe, and effective way to “reboot” the muscle without the risks of tissue-degrading cortisone or the trauma of hypodermic injections.
We are conveniently located to serve Setauket, Port Jefferson, and Stony Brook:
Messina Acupuncture 100 N Country Road, Setauket, NY 11733
Ready to release the tension? Contact us today or call (631) 403-0504 to schedule your consultation.